Almost Half of US Adults Have High Blood Pressure According to New Guidelines
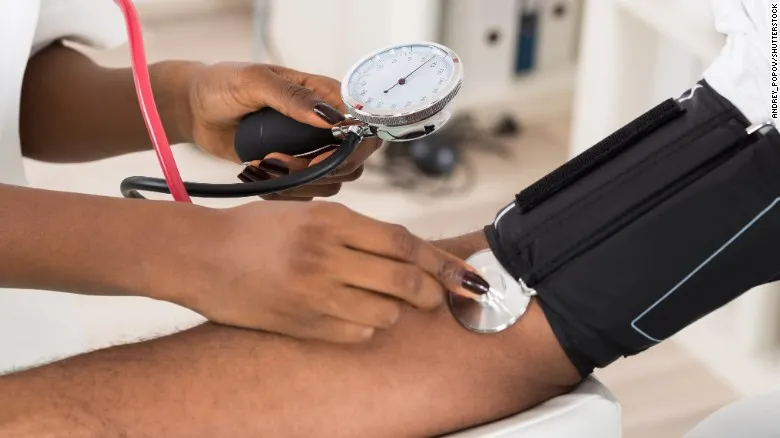
Prevention is always better than cure, and if that old adage holds true then the new guidelines for high blood pressure might just save countless lives. For many people, high blood pressure has become part of daily life. Millions of dollars go into the medications needed for this disease, but there’s no real cure unless you catch it early on; which is what the new guidelines aim to do: provide methods for doctors to detect, treat, and effectively prevent it.
Here’s how it goes.
If you get readings with 130 as the top number and 80 as the bottom, you are officially considered to have high blood pressure. This is a pretty significant change from the previous 140/90— which used to cover about 32% of the adult population in the US. With the change implemented, however, nearly half of the US adult population can now be labeled as having high blood pressure. For those who have less than 120/80, they are still considered normal, but anything above that is considered elevated.
So, why the change?
The idea is simple. These new guidelines were designed as a means of helping people take control of their blood pressure early on, giving them enough time to treat the problem and avoid the worse. This is in response to the widespread epidemic of hypertension—the major trigger for stroke and heart disease, which are just two of the leading causes of death in the world. After all, treating an illness can only do so much. What we have here is a solution that tackles the root of the problem.
Kenneth Jamerson, M.D., Ph.D., a professor of internal medicine and hypertension specialist at the University of Michigan Health System says, “Yes, we will label more people hypertensive and give more medication, but we will save lives and money by preventing more strokes, cardiovascular events, and kidney failure.” Jamerson is just one of the 21 experts given the task of changing the guidelines to suit the current health conditions worldwide and he believes that “if you are going to put money into the healthcare system, it’s to everyone’s advantage if we treat and prevent on this side of it, in early treatment.”
With these new guidelines, come new recommendations for maintaining proper heart health and preventing the onset of heart-related issues. Here’s what you need to keep in mind:
120 / 80
This is considered to be normal blood pressure. The committee suggests that you continue making healthier lifestyle choices and keep up with yearly checks.
120 – 129 / 80
This means you have elevated blood pressure and must begin making healthy lifestyle changes. Watch what you eat and incorporate more physical activity into your daily routine. After 3 to 6 months, you should get your condition reassessed.
130 – 139 / 80 – 89
This is considered to be stage 1 of high blood pressure. At this stage, you should get a 10-year heart disease and stroke risk assessment. Should you get less than 10%, what you need to do next is make healthier lifestyle changes. As mentioned above, you need to start eating healthier and exercising daily as well. Get a reassessment after 3 to 6 months.
If you do get a number higher than 10% during your initial assessment, the recommendations are as follows: healthier lifestyle changes, coupled with medication and monthly follow-ups until you get your blood pressure under control.
140+ / 90+
Much like stage 1, this calls for immediate lifestyle changes as well as 2 different types of medication. You must also keep up with monthly follow-ups until your blood pressure is under control.
*Note that these recommendations do change on a case-to-case basis. It pays to visit your doctor for a professional assessment.
Does this mean that the added 14% included in the new guideline would have to take maintenance meds from now on? Not quite. Only about one in five will need to do so, depending on the results of their heart disease and stroke risk assessment. A much smaller number when compared to the previous guideline, which was released in 20013. Instead, the new guide wills doctors to focus more on outlining healthier lifestyle options for their patients. Aside from prescribing medication, the focus is placed on treating and preventing the disease using natural means—starting with the patient’s lifestyle.
The guidelines are set in place to alert people that they are at risk, but it is also there to give them an idea about what can be done. Lifestyle changes don’t come easy, but it should be the priority. Something that many adults tend to forget, given how busy and fast-paced modern living can be.
Recommendations for a Heart-Healthy Lifestyle
So now that you know you’re at risk, what comes next? Following the recommendations set by the new guideline, changes should be immediate. The easiest way to start is by looking at your current diet and reducing your consumption of salt. It’s time to incorporate more potassium-rich foods as well, including dark leafy vegetables, bananas, avocadoes, and potatoes.
Aside from minding what you eat, you should also consider losing a bit of weight (you will need to discuss this with your physician beforehand, of course), getting more physical activity daily, and quitting bad habits such as drinking and smoking.
This new guideline is the first comprehensive one in over 14 years. It emphasizes the importance of developing an understanding between patients and doctor’s offices when it comes to diagnosing hypertension and accurately measuring blood pressure. Doing so removes the risk of confusion and wrong diagnosis, which can put the patient’s health at risk.
Hypertension 101 – What You Need to Know
By now, you’re well aware of the dangers that come with hypertension—but do you really know what happens in your body because of it? Often referred to as a silent killer because it happens without any real symptoms until the damage has worsened, hypertension accounts for more deaths due to complications resulting in stroke and heart disease. It only comes second to smoking.
Hypertension happens when the pressure of blood pushing against our blood vessels becomes too much. This then causes our hearts to work harder in order to get the blood pumping, whilst the blood vessels become less effective. If this happens constantly, it can cause damage to the tissues inside our arteries and may even affect the heart and our circulatory system.
These new guidelines do come with their fair share of potentially controversial proposals as well. It suggests that people who are 65 and older should be given held to the same 130/80 even if those patients are younger. In fact, another guideline from 2018 also suggests that patients who are 60 years old and older should be held to a standard that falls below 150/90 BP.
Will this be beneficial? According to Robert M. Carey, professor of medicine and dean emeritus from the University Of Virginia School Of Medicine and vice chair of the guideline writing committee, it is beneficial and has been proven to be so by several studies conducted since 2015. The idea, he says, is to “escalate the treatment slower and monitor any side effects”.
The guidelines seem to mirror this, pointing to BP-lowering therapy as lifesaving. After all, it is among the few interventions that have proven to be effective when it comes to lowering mortality risks among the elderly. Under the new guidelines, people aged 65 to 74 should see an increase in their blood pressure rates by 13% for males and 12% for females. Allowing more room and time for these people to make changes in their lifestyles— regardless of age.
To put this into perspective, here’s an outline of how other age groups will be affected by the new standard BP measurements:
- For men ages 20 to 44, blood pressure rates could triple—up by 30% from 11%. Women from the same age group, on the other hand, can expect to see their rates double. Going up to 19% from 10%.
- For men aged 55 to 74, about three-quarters of them could potentially receive a high BP diagnosis.
- Hispanic and Black men can experience a 17% increase in their rates, whilst Asian men will get a 16% increase.
Understandably, there are people who might feel a bit intimidated or even scared by these changes. It is important for people to understand that the changes and recommendations were designed to help. They were set in place to help doctors determine who might be at risk and what they can do about it.
Going back to the 10-year risk assessment, the doctors are urged to use a risk calculator to ascertain a patient’s risk of stroke and heart disease. This assessment coupled with the other recommendations provided in the guideline will open up communication lines between patient and doctor.
It provides patients with the chance to ask their doctors about the percentage of their risk and what can be done to lower it. Whether that be medication or lifestyle changes—or even a mix of both. The bottom line here is simple: the patients should be receiving ample explanation about their condition, whilst the doctors should be considering risk as they go through options for treatment.
Only then can they get to an accurate and effective solution that best suits the need of their patients.